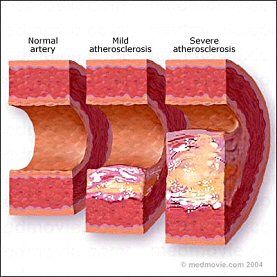
Description
The risk of developing coronary heart disease depends on multiple factors that are related both to lifestyle and genetics. Inherited factors account for as much as 30–60% of the variation in risk. Common genetic variants in more than 27 genes are associated with coronary heart disease. Although the ability for single genetic variants to predict risk is low, the variants can be summated into a score, to predict risk similar to other established risk factors.1
This genetic risk score has identified individuals at increased risk of coronary heart disease across both primary (without proven disease) and secondary prevention (with proven disease) populations. People with high genetic risk scores have the largest relative and absolute risk reductions with statin therapy.
Whilst statins are considered to be effective in secondary prevention, in primary prevention their role is less clear. The number of patients needed to treat (NNT) is between 66 and 104 to prevent a single event, in primary prevention. Contrarily the number of patients needed to harm (NNH) is between 65 and 255 for the lifetime risk of statin induced diabetes.1,2
This genetic test can be used in situations in which optimisation of the number needed to treat is relevant, such as in the primary prevention setting. This test can be used in conjunction with a statin metabolism genetic test to predict myopathy risk and optimise dose.
Download an information brochure here.
- Mega, J et al. Lancet. Volume 385, No. 9984, p2264–2271, 6 June 2015
- www.thennt.com/nnt/statins-for-heart-disease-prevention-without-prior-heart-disease/